Luckily I have not spent much time truly on the other side of the bed as a patient. And those moments have been brief, though worth being snapshot vignettes in this post.
There was the time at 18 years of age that I had surgery on my tail bone. When I went to the post operative exam, the surgeon had three medical students shadowing him that day (males all of them, not much older than I). The nurse put me in a room, noting I had sweat pants and a t shirt on and would not need to change to a gown. When the surgeon and his students entered, there was a brief exchange:
“How’re you doing?”
“I’m fine. Can I go back to work?”
“”Well, let’s see, bottoms up!” he exclaimed as he tipped me into leaning over the exam table as he pulled down my sweat pants, exposing my surgical incision (and buttocks) to the students. To this day I wonder. Was he doing a bravado thing for the students? Was it an attempt at funny, with me included and not as the object?
A few years later, when I was in grad school, I was hospitalized at UC Berkeley with a pneumonia. I was 21. Thought to be a bug called mycoplasma, the treatment those days was tetracycline. That stay was notable for several things. Because the hospital was right on campus, friends could visit at all hours- and bring me things I needed, like cigarettes. In those days the only reason I could not smoke in the room was because I was on oxygen. Can you believe it, pneumonia and no policy against smoking? You could often find me leaning out the window with my oxygen off, having my smoke.
While there, my face, arms, chest and back all broke out in the most amazing case of an acne like rash. It hurt, it burned, and it itched. None of the doctors seemed concerned, though they would say “Hmmm, I wonder” or “Hmmm, have you been sweating a lot when your fever breaks?” I was a relatively compliant patient (other than the smoking), sitting there, taking what medicines they gave, asking very few questions. There were also had medical students on a “student health” rotation from UC San Francisco. One day, in came the attending doctor, white coat pocket’s full of papers and gadgets. With him were 5 young men. Yes men…few women yet. They had on short white coats, with pockets stuffed more that those of the attending doctor. By the time of this incident I was very close to the same age as them. Most medical students went straight from college into med school.
They circled the bed with the attending at the center looking at me from the foot of the bed; the students, two or three to each side, were at his side with “What new exciting thing will I learn” expressions on their eager faces. I, the specimen, was asked to raise the head of the bed and sit up. This was not hard (I mean, really, I had just been at the window, hanging half way out to satisfy my nicotine urge). I complied. While they did not have beards and those big white collars, I could not help but think of Rembrandt’s The Anatomy Lesson of Dr. Nicolaes Tulp. I almost laughed out loud. If I had any inkling I would be heading for medicine, I might have been more understanding, but no, I was going to be a social policies person, community advocate extraordinaire. So these fellows amused me with their devotion to, well I was not sure what.
As the attending spoke about my case with words that were at that time a foreign language, he reached across the bed and with aplomb, he pulled down my gown, dropping it at my waist. There I was, sitting, at age 21, bare breasted with this horrific acne like rash, facing these eager students and their teacher as he lectured about my skin condition, tying it to the fevers and sweats I had in the previous days. This monologue was probably only a couple of minutes. It felt like an eternity. I sat there dutifully.
We teach differently and hopefully our students and residents know to attend to patient comfort.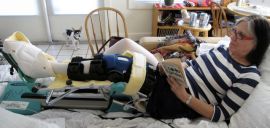
This is me, 2009, fractured tibial plateau, post repair by a surgeon who held my hand while they put me under anesthesia. I cannot tell you how much that meant to me.
Knowing that there is so little I can know about another’s experience is one thing; life reinforcing that knowledge hits it home.
All the time, I start patients on lisinopril and other medications that are called ACE Inhibitors. Some significant proportion of them come in saying, “Change it. The cough is unbearable.” When they say “cough,” I am all over it. I change their medication to something else. I ask questions about the cough to convince the patient and me that the cough is not from an illness rather than a side effect of the medication. I ask about fever, cold symptoms, smoking, sputum production, timing of the cough, things that make it better and worse. Inevitably the patient has stopped the medication and the cough has vanished, poof, just vanished. That’s enough for me; I suggest an alternative.
This past month my doctor and I have been discussing my blood pressure. From the 14 hours I could tolerate the 24 hour blood pressure monitor, it was clear.
OK first, to any of my patients who I have subjected to a 24 hour blood pressure monitor, my heartfelt apologies. I thought it was a nifty high tech device that silently and unobtrusively recorded blood pressures as the day went by. NOT. It is a clumsy cuff with a big fanny pack to be worn. I was more or less ok with that. BUT it beeped every time it was going to take a blood pressure, leaving me explaining it to co-workers and then awakening every 20 minutes during the night, to finally throw it across the room at 2AM. I thought I would have a hypertensive crisis from wearing the thing.
My results were clear: to manage my blood pressure all I needed to do was not work and spend a lot of time in bed. I like that idea, but I could picture the bills mounting, so opted for a very tiny, almost homeopathic dose of lisinopril, 2.5 mg for any of you who might be in the guild.
Sweet, I thought. Days 1 and two went fine and I even remembered to take the pill. I was getting over a cold and was not surprised by the occasional cough. (For those who do not know me, I do not any longer hang out windows smoking; I quit 28.5 years ago, but am sure, when I have a cold, that my lungs remind me of those days.) Then came day three. At about 1030 that morning I felt a tickle in my throat. No big deal. A tickle is a tickle. Thing to do: clear my throat. I coughed once and went into this several minute spasm that went from gasping for air to wanting to reach down and tear the tickle from my throat to knowing that some more coughing would not solve it. With a drink of water, it settled down. At 2PM there was a repeat, and again at 5 and 9PM. The next three days were no different. NOTHING prevented them; this was like nothing I had ever experienced, even in my smoker’s cough or whooping cough days.
I stopped taking the lisinopril and still need to tell my doctor. That very weird cough is gone. The real test would be to take it again and see if it has come back. I actually have suggested that to patients with whatever med they are not tolerating, to prove to them (and me) that it really was a side effect to the medication. I did that with tetracyline. Guess what: same rash, I am allergic to it. With this lisinopril, I am not sure I want to take my own recommendation.
What I cannot believe is that I have never really understood from what patients described to me that this cough is really beyond annoying. There is no way I could see patients, teach or even concentrate with it!
The last of recent lessons has to do with cataracts. I have probably had over a thousand patients get cataract surgery, almost all very very happy with the results. NOT ONE has talked about the 5 weeks of 4 times a day drops (four different ones, spaced 5 minutes a piece) Have you ever tried to do something and know that in five minutes you have to do drop #2 and five minutes after that drop #3 and after five minutes later drop #4…only to repeat 4 times that day? That requires a lot of focus.
And not one person talked about the challenge of how do you see when you cannot get your new prescription for six weeks? My surgery on my right eye was a piece of cake. For the first time since age 13 I can see 20/25 without glasses. Cool. Here’s the catch! I cannot read anything out of it. If I put on my glasses, my left eye is happy and can see mid, far, and near. For my right eye nothing is right. I have to wait six weeks to get that script. If I have my glasses off, my left eye is not good at near, mid, or far distances, but my right eye can see far. How did I not know this from all our patients? I am fine. My brain has adjusted and luckily I have not had a complex tear to repair for a woman having a baby or other need for both eyes to work together. Tomorrow I get a pair of glasses that will be right for both eyes until the left eye is done and then I will have six more weeks.
To my patients: I now know better how to ask about your experience. And I celebrate your resilience and how your carry on and adjust, regardless!








 The tests on the fetus did not show any chromosomal or structural abnormalities. There were neither knots in the umbilical cord nor anything abnormal about the placenta. Now you are pregnant and nervous. In fact you have so much anxiety that you want to have a Doppler machine (the little machine that lets you hear heart tones) so you can hear the heart tones whenever you feel anxious, to calm your fears. A prescription was not given to you because it was not felt to be medically necessary. This has been upsetting you and your anxiety increases.
The tests on the fetus did not show any chromosomal or structural abnormalities. There were neither knots in the umbilical cord nor anything abnormal about the placenta. Now you are pregnant and nervous. In fact you have so much anxiety that you want to have a Doppler machine (the little machine that lets you hear heart tones) so you can hear the heart tones whenever you feel anxious, to calm your fears. A prescription was not given to you because it was not felt to be medically necessary. This has been upsetting you and your anxiety increases.








